Symptoms, Causes & Treatments of Temporomandibular Joint Disorder
There are many conditions that dentists can help treat aside from just those that affect the teeth. For example, issues with the function of the jaw are often diagnosed and treated by dentists and maxillofacial surgeons. Such is the case with a condition known as Temporomandibular Joint Disorder, which can lead to a wide range of physical symptoms in the patient.
When thinking about the treatments that dentists provide to their patients, most people generally picture those that are most directly related to the teeth and gums. Things like teeth cleanings, cavity fillings, whitening treatments and fluoride applications, for example. However, these are just a small sample of the wide range of services that dentists can provide to improve the health of your mouth, as well as your overall well-being. This includes diagnosing and treating potential issues with the function of the jaw, and the joints that allow it to move properly for eating and speaking.
One such issue is known as TMD, or Temporomandibular Joint Disorder. This condition affects about 10% of the population, and its symptoms can vary widely in severity, so many cases go undiagnosed. To understand how TMD adversely affects a person’s health, we must first explore the structure and components found in the temporomandibular joint of the jaw.
What is the Temporomandibular Joint?
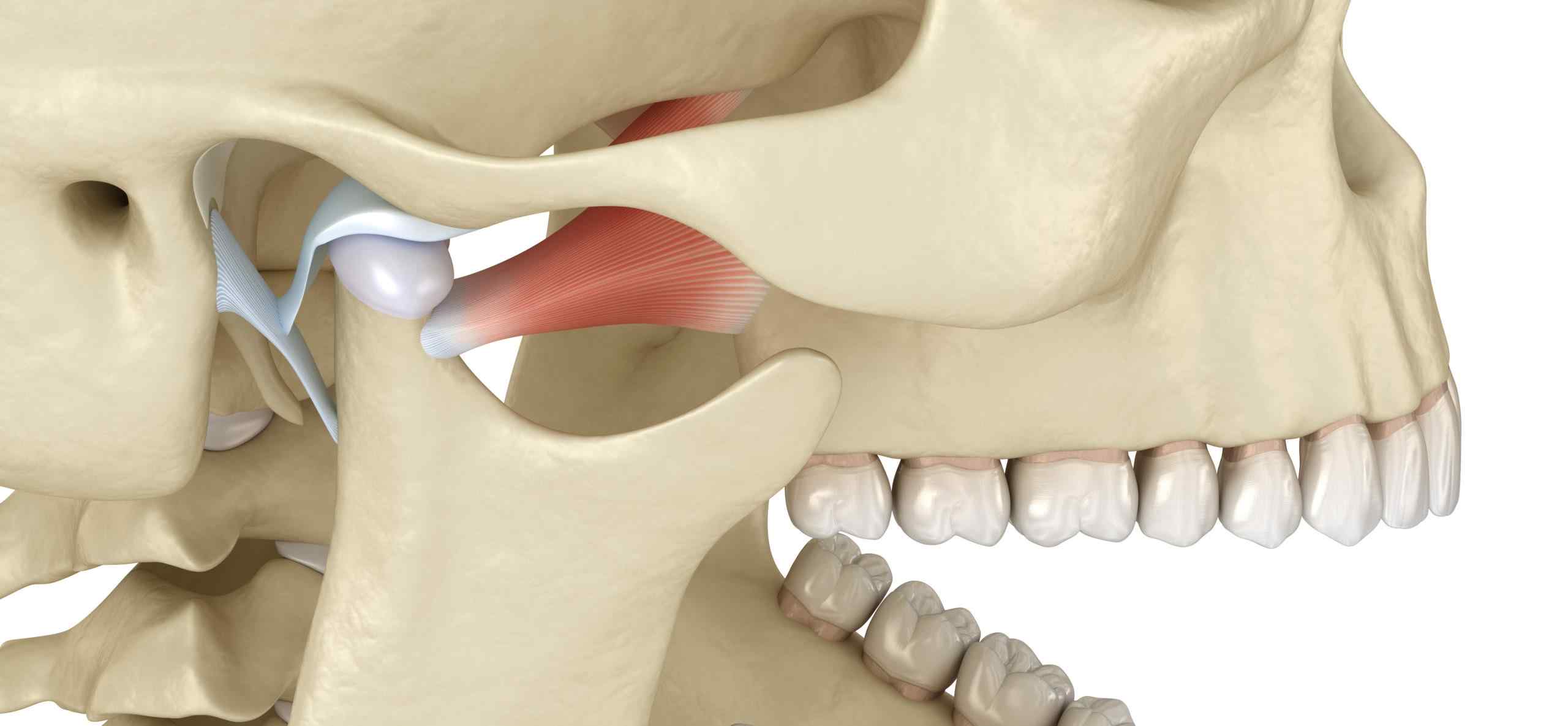
There are actually two temporomandibular joints (TMJ) in the jaw on either side of the head where the movable lower jaw bone, known as the mandible, attaches to the skull. The bones of the sides of the skull, known as the temporal bones, are shaped in such a way that there is a recessed socket where the lower jaw bone fits snugly. The temporal bones and mandible are joined by a series of ligaments and muscles, with the contact surfaces of the two bones separated by a smooth cartilage disk to allow ease of movement.
The temporomandibular joints are unlike most other joints in the body due to their incredible range of motion. The structure of these joints allows the jaw to move up and down, side to side, forward and backward. The jaw may move in any direction along these planes of movement as far as the ligaments and muscles will allow, allowing us to speak, eat, and drink with ease. When the movement of the jaw joints is irregular, it can result in the condition referred to as Temporomandibular Joint Disorder.
How Does Temporomandibular Joint Disorder Occur?
TMD occurs when the joint does not function properly and the bones, muscles, ligaments, tendons, cartilage and nerves move out of position and become misaligned. If this occurs frequently, it can manifest in a wide range of symptoms in varying degrees of severity. Some common causes of TMD include injury to the mouth or jaw from an accidental impact, nighttime teeth grinding or jaw clenching, misalignments in the teeth or bite pattern, or the onset of musculoskeletal health conditions such as arthritis and osteoporosis. When TMD does start to affect a person, the symptoms usually start out subtly. Over time, the subtle symptoms can become increasingly frequent, gradually worsen in severity, or both.
What are the Common Symptoms of Temporomandibular Joint Disorder?
If the jaw moves beyond the normal range of motion in any direction, it can cause several different effects. For example, tendons and ligaments may stretch beyond their ideal capacity, causing discomfort or soreness. Direct contact between bones can occur if the separating cartilage disk moves out of position. The nerves in the area can become pinched or compressed, creating numbness, tingling, or pain. Specifically, the physical symptoms a person with TMD may start to notice can include any combination of the following:
- Frequent unexplained headaches
- Discomfort or soreness in the jaw area
- Pain in the face, shoulders, neck, or eyes
- Noticeable clenching or grinding of the teeth
- Increasing tooth sensitivity
- Clicking, popping, or locking of the jaw
- Tinnitus (ringing in the ears)
- Light-headedness or dizziness
- Reduced jaw mobility
In the event that you notice one or more of these symptoms on a frequent or recurring basis, it would be wise to schedule an appointment with your dentist. They will conduct an examination and review your symptoms to identify the cause, and determine if you are in fact experiencing issues with your temporomandibular joint or if there is perhaps another cause. Symptoms associated with TMD should not simply be dismissed or ignored as minor, as there are long-term risks that can arise if the condition is left untreated and allowed to persist.
What are the Risks if TMD is Not Treated?
While the symptoms of temporomandibular joint disorder often start small, they typically continue to grow in intensity and frequency as time progresses. Eventually, this condition can lead to chronic pain and other health issues that must be dealt with.
Chronic Headaches & Muscle Tension – The most common effect of prolonged TMD is frequent headaches and constant tension in the muscles in the neck, head, back, and face. This relentless sensation of discomfort, soreness and pain in the head and surrounding areas elevates stress levels, reduces sleep quality, and can make it difficult to focus and function throughout your daily routine.
Difficulty in Moving the Jaw – As the jaw joint moves in and out of alignment over and over again, it can gradually lead to a situation where you may find the range of movement in the jaw has been reduced. As movement is restricted, it can hinder such functions as eating, drinking, and speaking. Some people may even find they have developed some form of speech impediment as a result of untreated temporomandibular joint disorder.
Accelerated Wear of Tooth Enamel – Constant tension in the jaw area often causes a person to subconsciously clench and grind their teeth, particularly at night. This grinding will increase the rate that tooth enamel wears down, making a person more susceptible to cavities and tooth decay, and possibly leave rough surfaces or sharp edges on parts of the teeth. Clenching and grinding of the teeth also contributes to headaches, muscle tension, and recurring pain in the head, neck, and face.
All of these effects can lead to other long-term health issues, so it is vital that the underlying cause of TMD be identified and treated so as to avoid these problems and improve the overall health and well-being of the patient. There are many possible treatments for temporomandibular joint disorder depending on the specific reason for the condition.
How is Temporomandibular Joint Disorder Treated?
The first step in treating the effects of TMD is to conduct a thorough investigation to determine the specific cause of the condition. This typically includes a physical examination, x-rays & dental imaging scans, and observation of the amount of motion the patient currently has in their jaw. Based on the results of this combination of tests, your dentist will be able to better diagnose the specific cause and develop a more effective treatment plan.
Common treatment approaches for temporomandibular joint disorder usually begin with non-invasive methods including physical therapy, relaxation techniques, massage, warm/cold compresses, and stress reduction. Ultrasound therapy is another popular approach, as the soundwaves work to stimulate the circulation in the area and naturally create a relaxing effect in the muscles. The idea behind these approaches is to relieve the tension and tightness in the muscles that are frequently to blame for TMD.
Sometimes the cause of TMD is related to tooth misalignments that result in a non-optimal bite pattern. For minor bite pattern problems, a dental mouthguard may be recommended that can be worn during the night to alleviate night-time clenching and tooth grinding. If the tooth misalignments are more pronounced, orthodontic treatment using braces may be a better option. Using braces to treat TMD has the benefit of also improving the visual appearance of the smile, which many patients appreciate as an added bonus. Most people who experience TMD see positive results from these non-surgical methods, however there are cases where a different approach is necessary.
In the event that dental surgery is deemed necessary, you may be referred to a maxillofacial surgeon if your dentist does not possess this particular specialist credential. However, if your dentist is a registered maxillofacial surgeon, then they will be able to perform the procedures necessary to correct more severe cases of TMD. The solution may simply be to relieve fluid accumulation in the temporomandibular joint using a method known as arthrocentesis, where the excess fluid is extracted with a needle.
In other instances, the surgical procedure may be a minimally-invasive arthroscopy that requires only small keyhole incisions to be made as the surgeon uses specialized tools to adjust the joint and reshape it as needed. For the most advanced cases, it’s possible that an open-joint surgery will be needed in order to provide the greatest access to the temporomandibular joint. This typically involves a longer incision to be made so that more significant adjustments can be made to the joint and its components to achieve the desired results.
What Should You Do if You Suspect You May Have TMD?
If you’ve been noticing any of the possible symptoms of TMD, the best thing to do is to book an appointment at Georgian Dental today and get your questions answered with certainty. Take note when you notice anything suspicious, such as unexplained soreness in the jaw area, frequent headaches, or occasional clicking or popping in the jaw when eating or speaking. This information will be helpful in diagnosing whether or not you are experiencing temporomandibular joint disorder, and will also help determine the best course of action to treat it.
Contact Georgian Dental today to arrange for an appointment. We look forward to seeing you soon!
Appointment Request
If you’re interested in any of our procedures, and would like to meet with one of our dentists to discuss options, costs and get additional information, complete this short form and we’ll give you a call to arrange for a no-obligation appointment at our Barrie clinic.