Oral Cancer Screening
Oral cancer screening involves testing people for early signs of cancer or precancerous conditions in their mouth before they have any symptoms. This could help find oral cancer at the initial stage. When abnormal cells or cancer is found at an early stage, it might be easier to cure, when there is a greater chance for a treatment. By the time symptoms arise, cancer might have begun to spread into other parts of the body. Our TotalCare philosophy at Georgian Dental® focuses on the all important early detection.
An Oral Cancer Screening includes an oral examination. This involves a search for suspicious lesions, including areas of leukoplakia (abnormal, unscrapable white patch of tissue) and erythoplakia (abnormal red patch of tissue). More than half of oral cancers have spread to the lymph nodes by the time they are detected.
Researchers are trying to better understand which individuals are more likely to get certain types of oral cancer. They also study the things general public do and the common things around us to see if they cause cancer. This information helps doctors recommend who should undergo oral cancer screening, which types of screening tests should be used, and how often the tests should be conducted.
It is imperative to understand that your doctor does not necessarily think you have cancer if he or she suggests a screening test. Some dentists may use additional tests to aid in identifying areas of abnormal tissue in your mouth. If a screening test result is positive, you may need to have more tests done to find out if you have cancer. If the dentist suspects a cancer, sometimes a referral is made to a specialist to assess the suspicious lesion further. Not only do regular dental checkups help keep your teeth and gums healthy, they can help detect oral cancer on time. Everybody should get a dental exam from a general dentist every six months.
The next time you visit your dentist, do not forget ask about an oral cancer screening. Your dentist will feel for lumps or abnormal tissue changes in your lips, tongue,cheeks, oral cavity, neck, head and thoroughly examine the soft tissues in your mouth, specifically looking for any sores or discolored tissues. Although you may have already been receiving this screening from your dentist, it’s a good idea to confirm that this screening is a part, and will remain a part, of your regular exam.
Each year in the United States, more than 30,000 new cases of oral cancer are diagnosed, and more than 8,000 people die of the disease, according to the Centers for Disease Control and Prevention. The five-year survival rate for oral cancer is about 50 percent. If it is not diagnosed and treated in its early stages, oral cancer can be deadly. Treatment for advanced stage oral cancer may lead to chronic pain, loss of function, permanent facial and oral disfigurement following surgery. The earlier the cancer is diagnosed and treated, the better the result.
What are the new technologies currently available for oral cancer screening?
There are broadly speaking, two categories of cancer screening technologies:
• Detection technologies
• Brush biopsy technologies
It is imperative to note that, the only ‘gold standard’ that exists to determine the exact nature of a suspicious malignant or premalignant lesion in the mouth is either a scalpel or laser biopsy. The detection devices as well as brush biopsy devices help create increased evidence that moves us toward carrying out the definitive biopsy NOT in place of it.
DETECTION DEVICES
Considering that current information may change daily, as of right now, the two primary/leading oral cancer detection technologies most commonly seen in the marketplace are ViziLite Plus and VELscope Vantage.
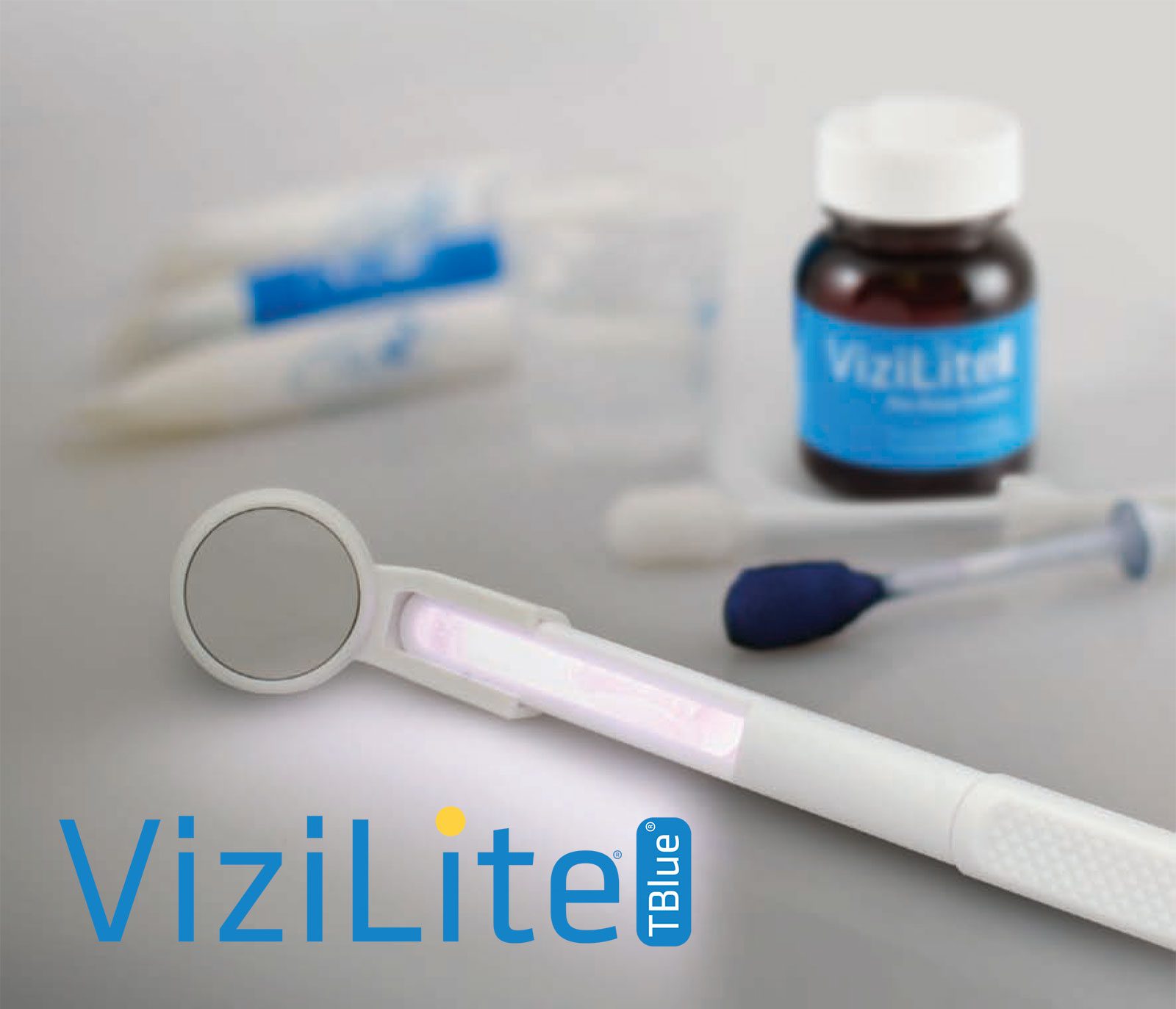
1. Vizilite
The Vizilite uses Direct Tissue Fluorescence Visualization (fluorescent bulb in hand-held device) uses an acetic acid rinse in combination with Chemiluminescent light or Speculite(chemically created illumination accomplished through a mixing of materials in a closed, thin, tube). The second is Direct Tissue Fluorescence Visualization (excitation and direct observation of natural tissue fluorescence).
Two other products on the market are MicroLux and Orascoptic DK which use the same basic approach as ViziLitePlus a mild acetic acid rinse and then a light source to visualize ‘acetowhite’ lesions.
Effectiveness
ViziLite Plus identifies suspicious white areas, but not red areas.
On the positive side, ViziLite Plus can bring to the attention of the clinician white areas possibly missed in their initial clinical examination. With ViziLite Plus, if a suspicious white area is detected, tol blue stain (T-blue) is then applied to mark the position of the lesion to assist the clinician to visualize the area under incandescent light.
According to the Summary of Safety and Effectiveness for ViziLite available on the FDA’s website,
“The marking system is not intended to be used as an indicator of lesions warranting further study, including biopsy. Whether a lesion is marked or not should not alter the clinician’s clinical behavior as dictated by the results of the Vizilite examination.”
The use of natural tissue fluorescence to help in disease diagnosis and detection (in the lung, colon, skin, cervix, oral cavity…) has been well studied and reported in the scientific literature over the past two decades. The fluorescence technique as employed by the VELscope system is thought to be sensitive to the involvement of all of the oral mucosal tissues from the surface of the epithelium down to the basement membrane and into the underlying connective tissue. When viewed through the VELscope handpiece, abnormal tissue typically appears as an irregular, dark area that stands out against the otherwise normal, green fluorescence pattern of surrounding healthy tissue. In addition to being used as a tool for the general practitioner to aid in the discovery of abnormal tissue, VELscope is also being used successfully to help clinicians to determine biopsy site selections and help delineate surgical margins around dysplastic and cancerous lesions.
Ease of use
VELscope is arguably more user-friendly when judged by the lack of pre-screening rinses and absence of restrictive time limits for use with any given patient. ViziLite Plus requires an acetic acid drying rinse prior to using the chemiluminescent light and has a 5 minute window of use until the ‘light’ created by the mixed chemicals goes out.
Patient acceptance
The increased cost factor and the need for a rinse that, to some patients is unpleasant, makes patient acceptance of the VELscope likely higher than ViziLite Plus. Controlled non manufacturer-supported studies need to be undertaken to clarify this point.
2.VELscope
i) Manufacturer: LED Medical Diagnostics Inc., Burnaby Canada
ii) Technology: This device utilises blue light excitation between 400 and 460 nm wavelength to enhance oral mucosal abnormalities by direct tissue autofluorescence. At these excitation wavelengths, normal oral mucosa is associated with a pale green fluorescence when viewed through a filter, whereas abnormal tissue is associated with a loss of autofluorescence (LAF) and appears dark.
Although pilot studies found that these excitation wavelengths could be used in vivo to differentiate normal oral mucosa from dysplasia, carcinoma in situ (CIS), and invasive carcinoma, the manufacturer extrapolated these findings to indicate that VELscope can help detect oral mucosal abnormalities not visible under white light examination.
Early research supporting the use of VELscope is comprised of case reports regarding its use on referred or review patients at specialist oral dysplasia clinics. Kois and Truelove found that VELscope assisted in the detection of dysplastic and malignant lesions not visible by COE and helped raise suspicion of lesions which would otherwise not be subjected to biopsy. In one particular case where widespread erythema was present, VELscope revealed an area which later proved to be a well-differentiated carcinoma. It also demonstrated its value in demarcating margins of established tumours where the malignant tissue extended beyond what was otherwise clinically visible. While the use of VELscope was in specialist environments, these case reports provided initial evidence that the device enabled clinicians to differentiate dysplasia from normal oral mucosa.
Disadvantage: VELscope has a fairly high rate of false positives, with reported specificities ranging between 15 to 81%. This suggests that VELscope is a poor differentiator between benign and dysplastic lesions. In particular, inflammatory lesions typically display LAF as well and, thus, act as confounders when using VELscope. As the majority of oral mucosal lesions seen in general practice are benign in nature, incorrect interpretation can lead to overestimation of oral mucosal abnormalities and patient harm through unnecessary referrals and biopsies.
VELscope’s main function is to serve as an adjunctive aid to rather than a replacement for COE. Lesions which displayed diascopic fluorescence were considered negative for LAF. Sensitivity was higher when VELscope and COE findings were combined than for either COE or VELscope alone, whereas specificity only increased slightly. This highlights the importance of clinical interpretation when using VELscope rather than relying on LAF on its own.
The authors also assessed the effect of diascopic fluorescence, whereby lesions displaying LAF return to a normal fluorescence pattern with the application of pressure. This technique enables clinicians to differentiate inflammatory lesions from neoplasia since inflammatory lesions typically display complete diascopic fluorescence, whereas neoplastic lesions do not. These results cannot be generalised to general practitioners as the study was performed by specialists, and advanced knowledge of mucosal pathology is beneficial to effectively differentiate between LAF and diminished autofluorescence.
Furthermore, Farah et al. observed that complete blanching of lesions was difficult to achieve and partial blanching could complicate interpretation. Therefore, VELscope is vulnerable to inter-operator variability.
Thus far, research on the use of VELscope for routine screening in the general population is limited. Huff et al.found an increased rate of detection of OED using VELscope in a private practice setting when compared to COE. However, this was conducted in parallel cohorts and the clinical characteristics of lesions discovered with VELscope were not discussed. It is unclear whether VELscope aided the detection of new lesions or helped raise the suspicion of lesions detected by COE. Consideration of a tested algorithm and decision making protocol would be helpful for general practitioners utilising the device. If the specificity of the device could be improved, there would be an increased scope for the use of VELscope in routine general practice.
The VELscope® Vx
The latest model release of VELscope technology, uses natural tissue fluorescence to discover abnormalities in the oral mucosa.
The VELscope® Vx system enhances the way practitioners examine the oral mucosa and screen for tissue abnormalities, potentially leading to the earlier discovery of precancer, cancer or other disease processes.
The VELscope® Vx system is a powerful device for the visualization of mucosal abnormalities such as:
- Viral, fungal and bacterial infections
- Inflammation from a variety of causes (lichen planus and lichenoid reactions, allergy to amalgam fillings, etc.)
- Squamous papillomas
- Salivary gland tumors
- Cancer and pre-cancer
- Other oral conditions
Unlike other adjunctive devices used by dentists, the VELscope® Vx system does not require any dyes or prolonged testing procedures. In fact, VELscope® Vx examinations can be performed in the dentist’s office during routine hygiene exams (and under normal lighting conditions) in about two minutes.
VELscope® Vx is also the global market leader in tissue fluorescence visualization; over 25 million VELscope® Vx exams have been performed by more than 12,000 dentists in 23 countries.
Indications for Use
VELscope® Vx is intended to be used by a dentist or health-care provider as an adjunct to traditional oral examination by incandescent light to enhance the visualization of oral mucosal abnormalities that may not be apparent or visible to the unassisted eye. VELscope® Vx is further intended to be used by an oral surgeon to help identify diseased tissue around a clinically apparent lesion and thus aid in determining the appropriate margin for surgical excision.
Other Oral Cancer Screening Devices available in the market are:
Identafi 3000®, DentLight D.O.E.™ and OralID
Appointment Request
If you’re interested in any of our procedures, and would like to meet with one of our dentists to discuss options, costs and get additional information, complete this short form and we’ll give you a call to arrange for a no-obligation appointment at our Barrie clinic.